
Get Your Free CRNA School Interview Prep Guide
Free CRNA School Interview Prep Guide Click Here
Whether you are currently practicing as an SRNA or are prepping for the future, learning about the induction of anesthesia will help you feel more prepared and confident at the head of the bed.
Today, we’re diving into what the induction phase looks like, as well as how to plan for an effective (and safe) induction of patients!
In this episode, we cover-
- How to create a comprehensive “game plan” for your induction ahead of time
- The differences (and overlaps) between general anesthesia cases and “twilight” inductions
- The importance of having all of your emergency supplies ready to go (Always have a plan A, B, & C!)
- Pacing yourself throughout the induction
- Key indicators for when you’re out of the induction phase
Happy listening, future CRNA! You’ve got this, and we’ve got you!
Get access to planning tools, valuable CRNA Faculty guidance & mapped out courses that have been proven to accelerate your CRNA success! Become a member of CRNA School Prep Academy here:
https://www.crnaschoolprepacademy.com/join
Book a mock interview, resume edit or personal statement critique:
Join us at the CRNA School Prep Academy Conference!
https://events.crnaschoolprepacademy.com
—
Watch the episode here
Listen to the podcast here
CRNA Clinical Tips: Induction Of Anesthesia
We are going to talk about induction of anesthesia. If you are practicing as an SRNA, this may pique your interest. If you’re thinking about becoming a CRNA, you may be interested to see what are some of the things that go into induction of anesthesia. If you’re a current student, you may have heard that induction is like taking off if you’re in an airplane. Some of the most critical parts of a case can be induction and emergence because that’s when a lot of things can go wrong in anesthesia. Usually, once you’re in the maintenance phase, you’ve smoothed things over. It’s like being up in the air in an airplane. That’s how I think of it anyway, but let’s go ahead and start from the top.
Planning Your Induction
Essentially, when you plan your anesthetic induction, there are some things you need to initially start thinking about and come up with a game plan on what you’re going to do. First and foremost is your patient and their history. That’s one of the first things you’re going to dive into is getting to know your patient and some potential areas of concern. Are they at risk for aspiration? Do they need a rapid sequence? Do they have a low ejection fraction of their hearts? Maybe we have to do a gentle induction.
I had a patient that had a VSD and I made sure I looked up the echo report to see whether this VSD had gone away and it had. Some VSDs, which are usually a left-to-right shunt, go away by age 2, or maybe even 4 years of age. If it doesn’t, then you can always do some interventions, but knowing the left-to-right shunt is not as dangerous as a right-to-left shunt because the left-to-right is where you’re remixing oxygen and blood with the oxygen and blood versus a right-to-left shunt, which is on oxygen and blood going straight into this body, and the system usually causes more problems with hypoxia and things like that.
We’re not going to get into that, but I’m letting you know that those are some of the things where you want to be investigating and knowing more thoroughly. For example, if your patient has a history of GERD, you have to make sure you’re asking, “Do they have any symptoms of GERD? How well controlled is it?” Same with like asthma. Some people list asthma in their history, but they may only take an inhaler as needed versus an asthmatic who takes it around the clock every day.
You need to know these things. Knowing things like if they’ve had a recent respiratory cold that in your mind says, “This person is at higher risk of bronchospasm during induction. What can I do to prevent that from happening or how to decrease the risk of that happening? That’s what I mean. You need to dig into the patient’s history to come up with a game plan for your induction of anesthesia. That’s the first thing you want to be aware of.
The Type Of Case You’re Doing
Next, and it goes hand in hand with number one, is what type of case you are doing. Depending on the type of case you’re doing, it’s going to change and tailor the type of anesthetic induction you’re going to do. Starting an induction for an open heart is very different than starting an induction for, say, an AV fistula. They both have considerations to take into hand. One would be a general anesthetic within a tracheal tube. Now, if you’re doing, say, maybe a mini AVR open-heart case, you’ll be doing one lung ventilation potentially. Therefore, you’d have to plan for that.
If you’re doing a case for an AV fistula, those are typically done under MAC, which is a monitored anesthesia care type of case. That’s what I mean that induction anesthesia looks very different for those two cases. Knowing your case and what to expect from the case plays a vital role in preparing for your anesthesia induction. If you’re a current student, you probably know the word Jaffe. In fact, it probably hunts you in your dreams as it did mine as a student. It’s a very thick book of surgical procedures and it gives you an anesthetic viewpoint on how to manage the anesthetic through those particular types of procedures.
For example, a weight crani is a very different anesthetic than a trigger finger. Every anesthetic can be tailored uniquely to the patient’s needs. I get people who say, “Is anesthesia boring?” I don’t think that’s boring. In fact, that’s very mentally stimulating to always be on your toes and think, “How can I tailor this anesthetic to this particular patient and case?” Not only are you taking into consideration the case, but you’re also taking the consideration the patient’s unique, maybe physical health into consideration as well. No two lap appy are going to look the same because the patient is different. One of the fun things about anesthesia is that you get to tailor every individual anesthetic you deliver to the patient’s needs.
Anesthesia induction is like taking off if you're in an airplane. Share on XThat’s the second thing that considers what case you’re doing. You really change and shift your type of induction. Based on the type of case, it leads you to, “Am I doing a general or am I doing a MAC case?” Some people call MAC, Twilight anesthesia. What I can say is generals, you can have a secured airway or a non-secured airway. In fact, a lot of monitored anesthesia care cases or Twilight anesthesia cases truly are generals, but if you look at the definition of a general anesthetic is loss of consciousness and not being able to respond to stimuli. I can tell you from working at a surgical center that did a lot of MACs or Twilight anesthesia cases that they were truly generals without an airway.
I encourage you to first recognize that. With every type of anesthetic you do, you always want to be thinking of a plan A, B, and C, and maybe even further than that. You want to always be thinking, “If this doesn’t go or if I need to intervene because this is not going to work, what would I do next?” If this patient has this in their history that may be because of this potential complication, what can I do preemptively? Always the best outcome is preventing something from happening. That’s always how you should be trying to think. “How can I prevent this?” You don’t want to be dealing with something after it happens. However, you still have to think, “If this does happen, what would I do?”
General Induction Versus Twilight Induction
I encourage you to always take that approach when you’re assessing every single anesthetic you do. I promise you that if you can do this routinely, you are going to be able to react quickly and be prepared for anything that can fall onto your plate during the anesthesia and wake up emergence, all of that. I’m going to ask you and if you’re an SRNA and you’re reading this, do you know the difference between a general induction and a Twilight induction?
My question is, “How do you know you’re through the induction phase when you’re doing the Twilight?” Think about that a little bit. I’ll give you my personal opinion on that. Again, this was from me doing a lot of those types of cases. For general anesthesia, it’s a much clearer picture of when you’ve completed induction versus a Twilight. Twilight could be a little gray.
General induction typically starts off with, if you’re working with peds, it’s usually inhalation induction, followed by an IV, and then you give IV adjuncts to aid in your induction. That could be Fentanyl, rocuronium, and maybe a little bit of Propofol or whatever they need via the IVs; Zofran, or Decadron. You start your anesthetic with Sevoflurane, for example, which is an inhalation agent that causes amnesia. That’s typically how you start those cases. That’s one type of general induction style.
You have a typical adult-style general induction that can be with an endotracheal tube or with an LMA, and that is where you give them oxygen debris to preoxygenate them. You don’t give anesthetic gases at that time because it stinks. The only thing that doesn’t stink as nitrous, but in adults, since they have an IV, you don’t have to bother with nitrous. You go straight to a 100% O2 because you have the IV.
You want to make sure you’re taking up their FRC, which is the functional residual capacity, which is the space in your lungs that you can fill with 100% O2. That will buy you time for apnea. It doesn’t mean that it’s going to control your ventilation. Remember ventilation is about CO2. This is going to control desaturation or hypoxemia. It’ll buy you more time to not desaturate as quickly.
In your time as an SRNA, you’re going to see someone who maybe has a big barrel chest or has a lot of weight up top. Maybe they’re apple shapes of some kind. They’re going to desaturate much more quickly than someone who’s pear-shaped because they’re going to have a lower FRC. You’re not going to be able to preoxygenate them as well as someone who is pear-shaped.
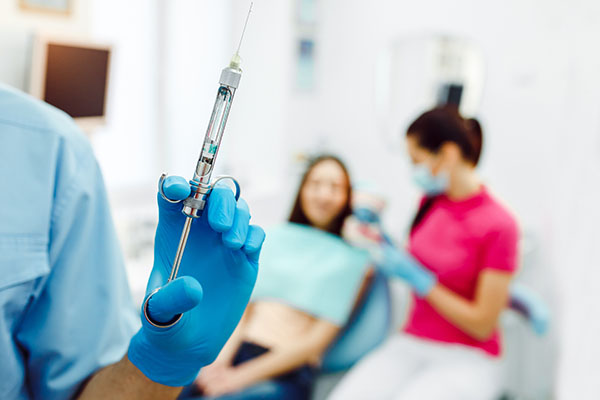
Anesthesia Induction: One of the fun things about anesthesia is the fact that you really get to truly tailor every individual anesthetic you deliver to the actual patient’s needs.
A way to overcome this, if this is your situation and you want to impress your preceptors, is to get a little bit of a ramp, and it can go a long way to decrease the pressure on someone’s chest. You can also set the head of the bed up a little bit, so keep that in mind when planning your preoxygenation ritual. Also, make sure you have a good seal. That’s probably one of the most common mistakes people make when they preoxygenate is they do not have a good seal. When you break that seal, you’re losing all that preoxygenation. You need a good seal when you’re preoxygenating. Ideally, you want to see your end-tidal O2 be above 85%. That’s when you truly have known you’ve done a good preoxygenation for your patient.
Back to a general versus MAC induction. With a general induction, you’re pushing IV drugs, and then essentially, how you know you’ve surpassed the realm of consciousness is one thing that you’ll see routinely done as you check for eyelash twitches. If you graze someone’s eyelashes with your finger, you’ll see their eye twitch. That’s a signal that they’re not completely induced yet. They need more time.
What’s fun about IV induction is you get to see their circulation time. Circulation time is the time it takes your body to pretty much circulate your blood in your body. That correlates with how quickly your blood, from when you’re injecting the anesthetic, reaches your brain because of the amnesia or analgesia-type effects. Someone who has a low ejection fraction, say 10% or 15%, is going to take several minutes to truly have an IV induction.
If you still have an eyelid twitch, and you still you’re like, “They need more,” and you keep giving more Propofol, then you could hurt the patient because now you’ve overdone it. You didn’t give yourself enough time to truly let those meds kick in and do their work. You would be surprised at how little it takes to do a true induction or to knock out someone’s recall. It does not take much. You have to take their age into consideration, but I’m letting you know, if you’re not patient with your IV induction, you could overdo it and give them too much Propofol, and then you’re dealing with hypotension. It’s not a fun way to start a case ever. It’s not good for the patients.
Make sure you’re being patient with someone who maybe has a slower ejection fraction and giving the IV drugs time to get to the brain. What you will notice when you do an induction in a healthy teenager who’s nervous and tachy away at a heart rate of 130. They’re all ramped up. They’re going to go to sleep much quicker because they’re going to have good circulation time.
You can always play a game with them and say, “Let’s count back from ten and see how far you make it.” Usually, it’s within ten seconds they’re already asleep, give or take. Sometimes they reach 13 or 14, but for sure, within fifteen seconds, even young, healthy kids are asleep. When you’re in this weird phase where you maybe are a little more sedated but not quite under general anesthesia, meaning your induction’s not 100% there yet, you can turn on your anesthetic gas to help, and not a lot; like a 0.3% end-tidal of your gas to help knock out the recall a little bit quicker and make everything work together.
What’s nice when you do that technique, you’re not slamming tons of Propofol. If you give what you think you need, the Propofol, and turn on a smidge of gas, along with some Fentanyl, you’re going to have the amnesia and that induction’s going to be sped up by incorporating the anesthetic gas as well. I would typically do that after the patient’s getting pretty sleepy, even if they haven’t quite lost their lid yet, but I can tell they’re not as responsive to being talked to.
I would turn on some gas. I would start helping them and give them little, tiny gentle breaths. You don’t want to cram in giant breaths or anything like that. Let them breathe with you. Don’t overdrive them or anything like that. Let them breathe until the anesthetic has caused its induction, and then when they stop breathing, you take them over.
Knowing your case and what to expect from the case plays a vital role in preparing for your anesthesia induction. Share on XDon’t be afraid if you need to do a good jaw thrust or oral airway. Make sure you always have that set out. I didn’t cover that, but when you prepare for an induction, you have to make sure you have all your emergency supplies ready to go. That can be drugs, airways, and all those types of things. You want to make sure again that you have a plan A, B, and C. If you’re anticipating a glide because based on your patient history and assessment or an anterior airway, you need to make sure you at least have the glide in the room.
Maybe you’re like, “Let’s go and see what we see with the DL so we can document what we see, but I have the glide there and I have an oral airway on standby so that I can make sure I can at least mask ventilate.” As long as you can mask ventilate, you have an airway. It’s cool. Take your time. No need to panic and worry. If you can mask ventilate, you’re going to be okay. The patient’s going to be okay. Take your time. You don’t need to rush and potentially damage the patient’s teeth or, God forbid, you damage something on their airway and cause bleeding because you’re rushing.
As long as you can mask ventilate, you’re going to be able to take your time and tank them back up. Let’s say you start an induction, take a look with your DL, and you don’t see anything. Maybe you didn’t anticipate that, and now you’re starting to panic. You’re like, “I don’t see any airway. They’re desatting on me. I have got to try to get this tube in.” You’re getting flustered and panicking.
First, take a deep breath. It’s okay. “Could you mask them?” That’s what you need to start thinking: “Can I mask them?” Mask them, do an oral airway, or whatever you need to do. If you need a two-hand mask, do a two hand mask, whatever you need to do to mask the patient. Remember, an LMA is a great thing to have on your back in case you can’t easily mask ventilate.
Emergency drugs would include things like succinylcholine, in case you get a bad laryngospasm, and also things like atropine in case you get some severe bradycardia. Even in kids, I always have some Robinul there because a lot of times, when you’re doing this inhalation inductions, you can go to junctional rhythms. You can slow down much. In the pediatric case, bradycardia is severe. They’re dependent on their heart rate for their cardiac output. Robinul is also on our emergency backstanding kits. I wouldn’t say in adults, we routinely did that, but for kids, we do.
It’s something to think about as well, so have your backup meds, airways, nasal trumpet even, oral airway, or whatever you think you need. Have it within reach. It doesn’t mean you have to crack it open and have it ready but make sure you have it within reach so you can easily grab it. The last thing you want to be doing is ever turning your back on the patient. Don’t ever do that. You want things close by as you can easily grab and get them ready to go
Back to my question, as far as telling the difference between, say, a general induction and MAC or Twilight induction, as I said, for a general, you look for that loss of lid reflex, where you’re twitching. To spoil some big suspenseful thing here, it’s very similar to a MAC case as well. However, if you’re truly doing a MAC, you should always be able to be responsive. Meaning a true Twilight case knocks stimuli could potentially respond and answer your questions or at least be cognizant. Maybe they don’t remember, but it’s like being drunk essentially.
It’s a good comparison. Like you’d be drunk and completely blacked out and not remember what you’re doing, but yet you’re alive and doing these things that you won’t remember doing the next day, that you’ll regret. It’s like that where you’re going to have amnesia, but you’re still going to be awake and if you need to, though you’re not going to ever say, “Ouch. That was too painful. That hurt.” That’s the difference between Twilight and general anesthesia.
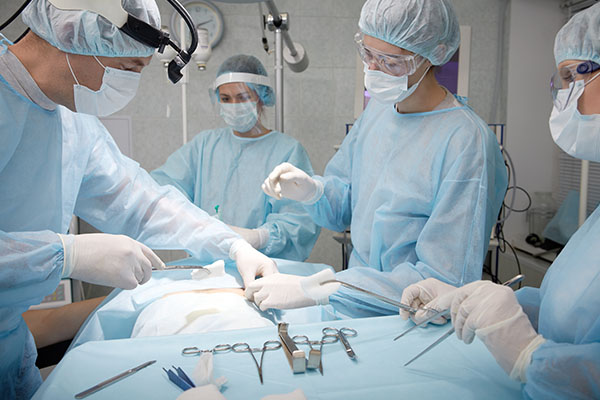
Anesthesia Induction: When you prepare for an induction, you have to make sure you have all your emergency supplies ready to go.
General anesthesia, you will not get that. It doesn’t mean the patient won’t move because they will. You have to have a MAC of anesthesia. Only 50% of the patients won’t move that knocks stimuli. Keep that in mind. Even if you have a solid MAC on and have amnesia, the patient gets stabbed with a knife. They’re still going to be like, “Ouch.” Their body’s going to reflectively pull away.
In a Twilight case, again, the patient who has a tracheal tube or an LMA in their throat they’re going to be able to vocalize, “I don’t like that.” They’re going to be able to tell you. What I can say is that the vast majority of the time that you do a Twilight anesthesia, what the surgeon likes or probably most anesthesia providers prefer is to have a heavy MAC. Meaning they’re not going to move on you. They’re not going to respond and knock stimuli. It’s like a general without an airway.
You have to be careful with this. Don’t get me wrong. It’s done all day, every day and it’s safe. It’s necessary. It’s good for the patient. You have to make sure that you’re on your A game because, in my opinion, it can potentially be a risk of your type of anesthetic.
Limitations To Twilight Anesthesia
Here’s the key, especially with the wrong patient in the wrong case. There are limitations to a Twilight anesthetic and there are limitations to who you can do this on. You can’t take someone with Pickwickian syndrome or severe sleep apnea and a BMI of 60. A little bit of Fentanyl can make them obstruct. You need to be very aware of what you’re working with here to know that you can deliver a safe heavy MAC. Make sure you’re keeping that in mind.
Also, another thing to keep in mind too is making sure, depending on the case, that you’re not overdoing it. For example, you could be putting a carotid stent in. Do you think you want a carotid stent patient to be completely out to where they can’t vocalize or tell you anything during the case? What happens if they stroke? If you do that, your surgeon is going to be so mad at you because now you’ll put the patient at undue risk. This is what I mean. You have to think about what is the case.
The thing is about those types of cases where you have to keep them a little more awake and they could have a recall- you cannot promise a patient undergoing Twilight anesthesia or MAC anesthesia that they will not have recall because the risk is always there. One of the best ways when I was in school that they described how to keep a steady state under Twilight anesthesia is when you have an infusion going, you’re delivering a steady state of drug. That’s the best way to create an even plane of anesthesia.
However, based on the stimulation going on in the case, your needs are going to change. If the case, all of a sudden, becomes more painful versus not painful, you’re going to react. If that steady state, the plane kept you comfortable during, say, the first half of the case, the second half of the case, maybe it’s a little more invasive and maybe they didn’t numb as good, a lot of Twilight cases go hand in hand with a good localization from the surgeon. Sometimes it’s better than others. Maybe they’re coasting along are doing great and you think they’re deep enough, and next thing, they’re like, “I felt that.”
The first couple of things, as an anesthesia provider, you’re going to get stares from the surgeon, who’s going to be like, “Make them comatose,” but you can’t do that and be safe. You have to say, “Can you please give more local? I will do my best that I can from my standpoint,” because it’s supposed to be a MAC. You don’t have a tracheal tube or taking over the respirations. They have to breathe. You have to be aware of how deep you can get them. That’s on the borderline of still being safe.
You cannot promise a patient undergoing Twilight anesthesia that they will not have recall because the risk is always there. Share on XA Mac is a truly tricky case to do versus a general anesthetic. It’s easy when their ventilation is controlled and their anesthetics more controllable. You don’t have to worry about it. You just paralyze them. It’s easier than having someone who you can’t paralyze and who you have to keep breathing. The Twilight can be a trickier type of case to do, but how I would judge whether I’ve finished my induction is the way those pieces tended to work is you get them in the room, start working in some drugs, whether that’s Fentanyl or verse, or you can do Ketofol.
There are different ways you can do your Twilight anesthesia. Ketofol where you mixed Propofol with Ketamine. If you’re worried about getting Fentanyl because maybe they’re at high risk of being sensitive to their CO2 or they already have sleep apnea, Ketamine is a great drug of choice because you don’t get respiratory depression with it as you do with Fentanyl.
Tailoring your anesthetic to the patient’s needs, back to that again, is what you will always continuously do. Sometimes you start a case and you think you’ve done a tailored anesthetic, and then you have to go to your plan B because now something else has happened. Either way, again, you want to make sure that you’re giving them a nice little cocktail. What I like to do too is I would give a little bit of Fentanyl or Versed if necessary. I would immediately put my Lidocaine in and turn my IV off and let that Lidocaine soak in the vein and create a mini little beer block or whatnot.
That way, when I started my Propofol infusion, the vein was nice and numb because Propofol can burn. If you’re pushing Lidocaine fast and it’s going right through the vein, it may or may not work that well. It still has sedative properties and still works as a good adjunct to your anesthetic, but as far as preventing the burning sensation from the Propofol, it does tend to work best the longer you let that soak in the vein. I’ve seen providers mix it.
Do you do what you think is best. Maybe play with different variations of this to see what you find works best. I encourage that, especially as a student. You let that Lidocaine soak and then you hook up the Propofol infusion as you’re getting them on the monitors and everything else, finishing, getting their oxygen on, and talking to them and letting them know what to expect. Make sure they’re comfortable.
Make sure you always do that. You never want someone to go to sleep when their neck hurts and then wake up with bad neck pain because you didn’t make sure they were comfortable in their current position. Never forget the positioning of the patient. That’s your job. You’re responsible for making sure they’re positioned so they’re not going to get an injury.
Essentially, I would always bowl the Propofol. How much you have to bowl is where your tailored approach comes into play and understand their history, what the anesthetic needs are, how painful the stimuli going to be, when is the surgeon in the room, and when is the surgeon going to be ready to cause more stimulation.
If you give them Propofol and the surgeon is not even in the room yet, while you’re going to have a period of apnea, you better be prepared. If they don’t come back breathing on their own, you’ve got to be prepared to put that mask on and help them breathe until they can come back breathing. Propofol is very forgiving. You will get them back breathing pretty quickly with Propofol, but depending on how well they’ve been preoxygenated, their FRC, their age, and overall health, you’re going to see a variation and desaturation. You don’t want that to progress to anything that could be life-threatening.

Anesthesia Induction: It’s easiest to go nasal trumpet in someone who is on the borderline of being awake than cramming the oral airway in.
Most kids don’t tolerate hypoxia. A healthy adult may tolerate a little bit more, but hypoxia can cause bradycardia. As I said, bradycardia in kids can cause a kid to lose perfusion and circulation. Know your patient population you’re working with and what you can get away with. Essentially when I’ve done a true induction with a Twilight anesthetic, if I say their name, call their name, they’re not going to respond to me. That’s how I know.
The next test I do is I maybe give a little bit of a painful jaw thrust. If you touch right behind your jaw, you’ll see your jaw move out, and it doesn’t feel that great. You can always test that and see if they start moving. If they start moving with that, you’re like, “They’re deep, but they’re not maybe deep enough for a real painful simulation.” you can always give them a little bit more when the surgeon is ready to cause more pain.
Once they’re localized and through that painful part because the localization hurts, then you let them coast. You can lighten them back up a little bit again and make sure they’re breathing and exchanging well. You want to be monitoring their end-tidal CO2. If they need an oral airway, give them an oral airway. If they need a nasal trumpet, give them a nasal trumpet. Just be careful. I would probably use some Afrin preemptively or spray a little bit of the end of it with some Afrin or Lidocaine jelly and stick it down their nose because you can cause a significant bleed with a nasal trumpet, so be very gentle. Make sure you’re picking the right size.
The worst thing you do is pick the wrong size and have to put another one in. Trust me, if the patient’s too light for a nasal trumpet, they’re going to let you know because it’s not fun to have something stuck down your nose in the back of your throat. That being said, it’s easiest to go nasal trumpet in someone who is on the borderline of being awake, than cramming the oral airway in because if you still have that gag reflex, that oral airway can gag you and make the patient cough. You have to be very deep for an oral airway to go in under a MAC anesthetic. I’m just putting it out there.
That covers the vast majority of induction types, styles, and maybe things to think about. I hope that it wasn’t too overwhelming for you guys because it is a lot of fun. It’s fascinating, keeps on your toes and the fact that we get to tailor it to your unique patient and case is fun. You’re going to have fun doing it. I hope you guys enjoyed this episode, please tune in next time. Make sure you go ahead and follow, like, thumbs up me, and all of that good stuff. I appreciate you. We’ll see you next time.
Important Links
Get access to planning tools, valuable CRNA Faculty guidance & mapped out courses that have been proven to accelerate your CRNA success! Become a member of CRNA School Prep Academy here:
https://www.crnaschoolprepacademy.com/join
Book a mock interview, resume edit or personal statement critique:
Join the CSPA email list: https://www.cspaedu.com/podcast-email
Send Jenny an email or make a podcast request!
Hello@CRNASchoolPrepAcademy.com
Join us at the CRNA School Prep Academy Conference!









