
Get Your Free CRNA School Interview Prep Guide
Free CRNA School Interview Prep Guide Click Here
Getting ready to start your open heart rotations? You’re in the right place, future CRNA! Cardiac pharmacology can be intimidating. With a number of different drugs (and possible patient reactions), there’s quite a bit of information to take in.
In today’s episode, we’re diving into an overview of commonly used cardiac drugs and how they work on a basic level to help you navigate your rotations with more confidence and knowledge.
** Disclaimer **
Nothing in today’s episode should be taken as absolute fact and it is up to the provider to confirm the correct doses and use of these medications.
Happy hearting, and enjoy!
Want access to numerous in-depth courses for navigating rotations? Become a member of CRNA School Prep Academy here!
https://www.crnaschoolprepacademy.com/join
Book a mock interview, resume edit or personal statement critique:
Join the CSPA email list: https://www.cspaedu.com/podcast-email
Send Jenny an email or make a podcast request!
Hello@CRNASchoolPrepAcademy.com
—
Watch the episode here
Listen to the podcast here
CRNA Clinical Tips: Open Heart Rotation Pharmacology Review
I’m coming on with a short disclaimer for this episode. We got pretty heavy into pharmacology in this episode, so I wanted to come on here and make sure everyone’s well aware that while I am sharing with you what I know to be accurate, that doesn’t replace the responsibility of you to confirm the accuracy of everything I go over. I also want to let you know that this is based on my personal experience practicing open-heart. It doesn’t necessarily mean it’s going to be your experience.
A lot of things we sometimes do, like anesthesia, are not necessarily going by the textbook. Some of this is opinion or preference-based practice. I encourage you to take responsibility for your practice and make sure you have a thorough understanding of all of these techniques and drugs so that way when you go into your open-heart rotation, you truly understand why you’re doing and making these choices, not just because you heard it on Jenny Finnell’s show. I hope that you guys enjoy this episode. Let’s get into it.
—
In this episode, we are going to go over a special area that I love, which is cardiac pharmacology. As some of you may know who have been around for a while, I have a background in open-heart anesthesia. I love open-heart anesthesia. My passion for this is there. I’m happy to share with you some of the knowledge I have gained over the years. I want to run through some down and dirty cardiac drugs with you.
I’m not going to go into the full pharmacology lesson plan for you. I simply want this to be an overview so that way if you are getting ready to start your open-heart rotation, you are familiar with some of the more common drugs that you will use in your rotation and maybe how they work on a pretty basic level so if someone were to ask you, they get the gist that you know what you are getting yourself into and that you understand what you are doing. That’s key when you start your specialty rotations.
You are not going to fly in there as an expert, and you shouldn’t expect yourself to, but you should have a good base and understanding of the types of drugs you are going to be using, the mechanism of action, some of the key side effects to look out for, potential things that you could come up if you are using those types of drugs, and also knowing how to dose them correctly. This is meant to give you a good overview of various cardiac medications. Keep in mind that no matter where you do your hearts, you are going to see a slightly different technique.
I can speak to what my experience is, but I also know from my training and talking to CRNAs who do open-heart at other hospitals that every system seems to have its own way. Some places routinely use nitro, and other places do not. Some places routinely draw up certain drugs while others do not. Some places practice opioid-sparing techniques, even an open-heart. I’m telling you all this ahead of time because it’s knowing that this may not be the standard based on where you go. I will go ahead and jump into what I’m familiar with and share with you what I know. Let’s start with some drugs.
When I do my cases, I would like to organize things in a way that I have my uppers, downers, and narcotics, so I have everything labeled and organized. I would even go to the extent if I had a syringe of neo and ephedrine. I make sure I label them differently, especially epi. If you have epi, neo, and ephedrine, they are all purple labels. Especially if something were to happen, you need something quickly. You have to make that choice about what drug you want to use. You want to make sure you have those labeled differently.
That’s one of the first pieces of advice I could give you. For example, epi typically was purple with a black line on it, but I’d put one sideways horizontally. I’d wrap it around the syringe. I had two purple labels on that syringe of epi. For my neo, I went horizontally with that one. For my ephedrine, I went around the base all the way around. All three purple syringes were labeled slightly differently, so I could easily pick them out if I were to grab them in a pinch. This is one way to make sure that you are being vigilant and safe.
You always still want to make sure you are reading your labels and checking things before you push anything. For me, that was one more double-check method that I used to make sure I was grabbing the right drug. The same thing goes if you have a couple of different types of narcotics or anything that has the same color label. You probably wouldn’t be surprised. We get label-fatigued. We have all these colors that we are used to, and the same with when you get medications out of your med drawer. You are used to seeing the Zofran with a green or blue cap. That can change. You have to be diligent and aware of when those things change.

Cardiac Pharmacology: The key when you’re pushing vasoactive drugs is to go slow. Go just little increments at a time. Pick one thing at a time. Don’t mix different drugs together.
Downers
When you have syringes with all these blue labels, you could think you are giving fentanyl, and you are giving Dilaudid based on how you have it diluted if they are in the same size syringe. When we did open-heart, we used Sufentanil. Make sure that you are labeling things so you can have a way to double-check yourself before you push anything. Once you push it, you can’t take it back. We are going to start with drugs, which I call downers because they bring your blood pressure down. The first of which is common is nitro. A lot of patients who even come to the OR who are getting ready to have CABG usually 5 mcg a minute, which is a low dose.
A nitro bottle comes as 200 mcg per ML in a bottle. Whether you are going to run it as an infusion or whether you are going to dilute it, you want to make sure if you are going to use it as an IV push that you are diluting this because 200 mcg per ML is a lot. How I would dilute it is that I would take 1 CC. You’d want to make 20 mics per, so you would dilute 1 CC with 9 MLs or a total of 10 MLs to make 20 mcg per. If that doesn’t make sense to you, what I do, my head math, that to me is easy, is I knock off zeros.
The easiest way I can simplify math is if I’m diluting something down 10 MLs, now you have 200. If you were across off (1 zero from 10ml and 1 zero from 200mcg) 0s, now you have 20 and 1, meaning you have 20 mics per 1 ML. For me, that’s the easiest way I can do that math in my head. I have also seen people dilute it down to 40 mics per ML. I like it at 20 mics per ML. It gives me more control of how I give it. Nitro is very quick on. It’s relatively short lasting. The half-life is 2 to 3 minutes for nitro technically based on the circulation time, the patient, and that type of thing. You can burn yourself. Think about if you need your blood pressure down, but you have two minutes where if you overdo it, now you are hypotensive.
The last thing you want to do when pushing any vasopressors or vasodilators is you don’t want the yo-yo effect. You don’t want up and then down. Sometimes it happens. You do the best you can to avoid that situation, but that’s not good for the patient. It’s also very labor intensive for you. Sometimes the more you get into that up-down scenario, the harder it’s going to be to fix that. It can be distressing, not only for the patient but for yourself and the whole surgical team involved because that’s not good. You don’t want up and down type of vitals. You want train track vitals. You want a steady line of vitals.
The key when you are pushing vasoactive drugs is to go slow, go in little increments at a time, and pick one thing at a time. Don’t mix different drugs together. I’m not saying I don’t ever give neo and ephedrine because sometimes I do, but be careful. You have to know how the patient reacts to those drugs before you do that together. Don’t initially go for neo and ephedrine because you don’t know how they are going to react. Once you can gauge their reaction, and trust me, all patients react differently to these types of drugs, then you can make that judgment call on whether you need to combine them to get the effect you want.
Initially, start small. I promise you won’t be in trouble if you start small and work your way up. You can always give more. You cannot take it back once you give it. The next drug I want to bring to your attention that, at least for me, was commonly used in open-heart was Cleviprex. This is also known as Clevidipine. This is a calcium channel blocker. Nitro is mostly a vasodilator, meaning it mostly affects the venous smooth muscle, whereas the Cleviprex is mostly the arterial smooth muscle. What’s good about the Cleviprex versus the nitro is you don’t get the venous congestion.
You can essentially change someone’s blood pressure without affecting their pre-load, which, if you understand the heart physiology, if someone’s already in heart failure, especially with the pump, meaning they are not pumping blood forward, and that’s the most common type of heart failure, the systolic dysfunction or the pump function, then you can worsen someone’s heart failure by increasing their pre-load significantly. Think about it. The blood is not able to go forward, so you are going to dilate that ventral even more. You want to be careful with pre-load. You can do more harm than good with it. Nitro can affect your pre-load where Cleviprex does not.
We typically didn’t use nitro routinely in our open hearts. Some places will put it on 5 mics a minute and let it run pretty much the entire time. If I were in a TAVR or something like that, where I would anticipate potentially an acute increase in my blood pressure when I got the valve in place, I would have nitro diluted ready to push. For the most part, in my routine open-hearts, I rarely ever used nitro. If I picked a drug of choice, it would be Cleviprex or Clevidipine to help lower my blood pressure. That goes on in the infusion pump. I would not recommend pushing that. I can’t say that people have not, but in my practice, it’s so quick to titrate that drip. It’s pretty easy not to have to draw it up as an IV push.
You can start it at 1 or 2 milligrams an hour and go up to a max of 32 milligrams an hour. There would be times when I would jump from 2 or 4 milligrams an hour to 8 milligrams an hour. Within ten seconds, my blood pressure was quickly adjusted because it was quick on. It’s quick off. It’s going to look white, like propofol. A lot of times, I bring my patient over on a little bit of Cleviprex, and the nurse will go, “You are still on propofol.” I’m like, “That’s not propofol. It’s Cleviprex.” They are both made out of that lipid-based medication. It looks white, but because of that, it’s quickly hydrolyzed by plasma esterases. It’s very quick on and quick off. The half-life is approximately one minute. Within one minute, half the drug is completely out of your system. It’s a great drug. It can decrease your SVR without affecting pre-load. That’s Cleviprex.
When you start your specialty rotations, you're not going to fly in there as an expert, and you shouldn't expect yourself to, but you should really have a good base and understanding of the types of drugs you're going to be using. Share on XThe next one I’m going to point out is Nipride. This is another drug, along with nitro that I didn’t routinely use in my open-heart, but it is out there, and some places will routinely string it up. They have gotten away from that because of how expensive it is. That’s my two cents on that because it is an expensive drug. It’s also very potent. This affects your arterials and veins. It’s a vasodilator. It’s potent. Essentially, how it works is it produces nitric oxide, and nitric oxide in itself is the dilator.
Here’s another thing you have to keep in mind with Nipride. This usually only plays into patients in ICU because the longer you are on it, the more risk you have with this, or at high doses is cyanide toxicity. Because of the metabolite, it can produce cyanide. If you are on it for a longer time, which is over 72 hours, like several days, you can have cyanide toxicity. It can be shorter than 72 days if you are on high doses of it. Patients with hepatic and renal impairment can have more significant complications from this because they are not able to adequately remove the metabolites from the Nipride drip.
When you are using Nipride, and if you are using it on your open-heart, it’s usually going to be temporary for the case itself. It may or may not go with the patient over to the ICU, but you start low. I would potentially start it low, like 2.5 mcgs per kilo per minute. The max is 10 mics per kilo per minute. I have never seen that get close on a patient. I can’t even imagine having that dose on a patient. They’d have to have some severe uncontrolled hypertension to be on that dose. With an open-heart, less is more. You always want to go low when titrating your drips and always work your way to what you need. I would start at very low.
That covers the three most common drugs I saw routinely in my open-heart to decrease someone’s blood pressure quickly. I’m going to throw it out there. Not all places will do this. Some places will probably frown on this, so please don’t go into your open-heart rotation and be like, “Jenny Finnell told me that this is what she did.” Make sure when attending your CRNA that you’re coming up with a good game plan on how you like to do things. Especially if it’s your first day or first week in open-heart, you should always be observant. Try to pay attention to what your CRNA is doing and pick up on those cues because that’s going to help guide you on how they like to do things. I would use gas.
In open-heart, you put them on ISO and let them coast at 0.6 end-tidal of ISO. That’s how you would run an open-heart case. Don’t get me wrong. I did like them there most of the time. You have to use your best judgment as a patient. How old is the patient? Are they a young person going through an open-heart versus someone who’s in their mid to late-80s? As you know, your metabolic demand is going to be different based on your age. Also, are you cooling the patient and warming them back up?
When you warm up a patient, you increase their metabolic need. You are going to have to adjust your gas accordingly, but we use adjunct midazolam versed. The risk of recall is low, especially if you have 0.6 ISO on and you are using Sufentanil and midazolam. It’s very low. Keep in mind that MAC-awake is 0.3, so you still have amnesia on board. If you think about what you are doing in an open-heart, you want to use enough gas-cause amnesia, but you want to control their vital signs with other drugs. That’s why we use vasopressors, opioids, and anxiolytics, which are that amnestic drugs. We are combining all these different drugs to create a perfect little picture for the patient because gas can be a big vasodilator, which is why sometimes I use it.
If we were in a pinch and I didn’t have Cleviprex strung and ready to go, and I didn’t have nitro drawn up and diluted, I would use my gas. I want to caution you about this because you have to be very careful with this. This can burn you. Don’t get me wrong. You have to learn the technique. Remember, when the gas is up, it flows up and down. You are not going to get the gas on as fast. Your flow controls the speed at which you get the gas on and off, meaning you can get the gas on and off pretty quickly. You have to keep your flow up if you are going to get the gas off quickly. I would increase my flows or my gas until I saw somewhat of a change in the blood pressure.
Based on how quickly they would drop in, I would either leave my flows up or turn the gas down. If they weren’t dropping very quickly, I would turn my flows down and the gas down. I let them hold on to that gas a little bit longer as they gradually coasted down. I would also be cognizant of it the entire time and be adjusting my flows as needed to either dilute the gas or go back up with the gas. That technique worked beautifully. It’s something that you have to learn how to do. I don’t suggest you go in there and try to do it on your first day. If you don’t see them doing that, I also don’t suggest you do that. If you see them doing it, embrace it and try to learn how to use your gas to control the blood pressure because it can come in handy if you’re in a pinch.
Positive Inotropes, Etc.
Let’s go ahead and get into some vasopressors as well as some positive inotropes. Inotropy is the contractility of the heart if that is not a term you are familiar with. A positive inotrope is increasing the contractility of the heart. If you have a negative inotrope, it does the opposite. One of the most common drugs you are going to use in the open-heart is epi. Epi affects both alpha and beta receptors. At higher doses, it affects more alpha than beta.
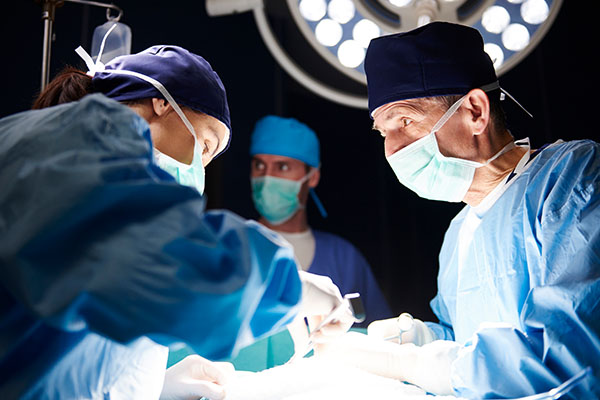
Cardiac Pharmacology: One thing you have to keep in mind with nipride, which usually only plays into patients in the ICU because the longer you’re on it, the more risk you have with this or at high doses is cyanide toxicity.
The beta is where you get the contractility, and the alpha is where you get the squeeze where you get the vaso-contraction. Based on what you are using it for, you can change the dosing. At lower doses, that can be a vasodilator and a bronchodilator because it mostly affects beta-2 receptors. We rarely ever use epi for vasopressor in open-heart. I routinely would use it as a cardiac dose, which would be 0.03 mcgs per kilo per minute. We didn’t titrate that unless based on the cardiac index, we knew they needed more. Even then, we would go up by a little 0.04. I rarely ever saw anyone get to a 0.06. That’s usually if things were not going well, but they would end up on a 0.06 dose. That’s even still very low.
If they ended up not doing well, we could take them up to the max dose. On a routine open-heart, for someone who had low cardiac output and needed a little bit of support, we teeter them on the line of beta-2 and beta-1 stimulation. It was still probably enough to give them a little bit of bronchodilatory effect, but also a little bit of beta-1 to help with contractility. The other issue with things like epi is it will increase your heart rate. Because of that, you are going to increase your O2 demand. That’s not necessarily good. You don’t want someone who already has poor heart function to have increased O2 demand.
You have to be careful with epi because it can worsen someone who already is not meeting their metabolic demand with the blood flow, oxygen, and things like that. We would use a small dose if we used it. You also want to remember someone who has a physiology like aortic stenosis. You don’t want to whip the heart. It’s what we would always say. It’s because they have a concentric hypertrophied ventricle. They don’t have a lot of filling space. If you are putting something like that on epi, they can’t fill very well because usually they are hypertrophied. Their chamber is smaller for having to overcome the increased pressure they need to object out of the stenosed aortic valve.
Epi is not a good drug of choice for those patients. Keep that in mind. A better drug of choice is Levophed. Levophed will give you a little bit of alpha and beta. It’s a little more forgiving with the heart rate increase. You can still see a significant heart increase with Levo, but not much, considering the low doses that we use. When I say low dose, it’s 0.02 or 0.03 mics per kilo per minute. We rarely ever went up above 0.08. If you are at 0.08 of Levo after an open-heart case, you need to be starting to think about what’s going on. Did one of their bypasses go down? It’s because that has happened.
I have seen a patient get moved over from the operating room table to their bed and have noticeable ST elevation. It turns out one of their graphs went down. That can happen. If you are ever at a 0.08 mics per kilo per minute dose of Levophed after open-heart, you have to be thinking. Look at their SVR. Are you over squeezing them? You want to be evaluating their SVR before putting them on a high dose of Levophed.
If they are vasoplegic and you need that squeezed, that’s okay. Make sure you are evaluating that. You don’t want someone who has an extremely high SVR, and you are at a high dose of Levophed. You are just squeezing when what they need is an inotrope. Their pump is failing. You want to make sure you are being cognizant of that because maybe they need some background epi with it and the lower dose of Levo.
My suggestion to you is to start Levophed off at 0.02 to 0.06 mcg per kilo per minute. I would start at a 0.03. I would start at 0.02 and work my way up to 0.06. The range I said with you is a very small range of Levo that we ended up needing. Assess, “Do they need fluid? Is it because they are dry?” You don’t want to keep squeezing someone who needs fluid. Always assess what’s causing the hypotension. Don’t start treating it and not knowing what’s causing it because you can do more harm than good. That is Levo. Next, we are going to go into vaso. Let me back up for a moment because I forgot to mention how you mix Levophed. I also forgot to mention how you mix epi. I figured I throw this in there.
It would be cool if I went through anesthesia math. I have a full course of anesthesia math inside CRNA School Prep Academy. It’s a couple of hours’ worth. If I did a down and dirty anesthesia mental math, it would help some of you because I promise you math anesthesia is not hard. It’s very routine. You do it all the time. It becomes simple, and I love simple. Mixing up epi and Levo, I promise you it’s not as scary as it sounds. How we did it is, for epi, we would put 4 milligrams in 250 MLs. Whenever you put any drug into 250 MLs, the math is super easy. I’m super excited to share this with you because it will blow your mind.
Instead of using some fancy way of doing math, if you put 4 milligrams in 250, 4 times 4 is 16. You now have 16 mics per ML. It’s that simple. You times all the milligrams. Whatever you put in 250, you times that by 4 of the milligrams, and that’s what you get in mcgs. If you are putting 8 milligrams of Levophed into a 250 bag, you are going to get 32 mcgs per CC. It’s that simple. That will always work. That’s only for a 250 bag, keep in mind. Those are nice, easy math for you guys. Let’s go back to vaso.
Make sure you read your medication labels and check things before you push anything. Once you push anything, you can’t take it back. Share on XVaso is a potent vasoconstrictor. It increases your arterial blood pressure. How it essentially works is it’s a hormone that is found in the hypothalamus. It’s sent to the posterior pituitary, which is where it’s released into the blood. It can work in your kidneys to help reabsorb fluids. It’s very potent. It’s an ACLS drug. You should be familiar with it.
How we would use it is you either put it on a drip or do an IV push. We would occasionally put on a drip. You don’t titrate it. Once it’s on a drip, you usually let it stay as the baseline rate. If you were to use it as an IV push, you dilute 20 units. You take 1 ML, which is vasopressin. You dilute it into 19 CCs of saline, which makes 20 MLs total, which dilutes it down to 20 or 1 unit per for a total of 20 units in that entire syringe. You would then push either 0.5 to 1 unit at a time. Always start small. Push that little half and see how they react because it’s potent. Some patients react well to vasopressin, and some don’t.
Vasopressin is the drug of choice if you have a patient who is vasoplegic from lisinopril or any of the pril drugs. It’s a great drug for that. Even if you are not in an open-heart case or you are in a case on an ACE inhibitor, vasopressin is a great drug of choice if they are not reacting to the neo that you’re giving. Keep that in the back of your mind. Be careful with it. You want to make sure you are diluting it correctly because it is very potent. You never want to not dilute that drug. You have to dilute that drug. Be careful with it.
If you are putting it in a 50 CC bag, you want to make sure you are putting 50 units in 50 CCs. It’s 20 units per, so you have to make sure in one of the vials that you are only taking a half CC from that to get 50 units to put in 50 CCs. That’s how we would dilute vasopressin when we are putting it on a drip. We are going to go into milrinone. Milrinone is a phosphodiesterase inhibitor. It modulates Cyclic Adenosine Monophosphate or cAMP. It’s a positive inotrope, but it also decreases your afterload. It’s a unique thing about milrinone that you can have both decrease in afterload and a positive inotrope.
Why it’s selected is, for the positive inotrope, not that the afterload is not desirable. What I will say, at least in an open-heart situation, sometimes patients won’t tolerate milrinone. Even though it is a good drug of choice for them, they don’t tolerate it if they can’t tolerate the decrease in afterload. It can be an epi drug, whether it’s going to tank their blood pressure or not. You have to go very slow with this. We would never bolus it. If you look it up in any textbook, it will say to give a loading dose. We would never do that because that almost always would cause hypotension. We would skip the loading dose and start it at 0.375 mcgs per kilo per minute.
That’s where we would leave it. We didn’t titrate it. We left it there. If the patient tolerated it, great. If they didn’t, we would have to stop it. That’s milrinone. A drug that I want to touch on that’s also very common other than the next most common drug, which I will get into last, is ephedrine. Ephedrine comes in 50-milligram vials. The dose per kilo is 0.2 milligrams per kilo. However, I still think that’s a high dose, especially now that I do a lot of pediatric cases. You always want to go low. Like I said before, you want to see how people are going to react. Ephedrine is one of those drugs where you never know what you’re going to get when you give it.
You could give 5 milligrams to good size adults and have a heart rate of over 100 from 70, or you could give 5 or 10 milligrams, and you could see nothing. Ephedrine is one of those drugs that you can quickly get acclimated to it. Over a period of time, you get sensitized to it, so you don’t react the same way. I have seen that happen where initially it works well, and halfway through your stick, it’s like you’re giving water. Ephedrine is one of those drugs that’s indirectly acting as a vasopressor.
It works on alpha and beta, but it ultimately works by inhibiting norepinephrine reuptake, which essentially allows more norepinephrine to circulate in the body. Meaning it increases your blood pressure. Norepinephrine is a natural catecholamine in your body that increases your blood pressure. That’s how ephedrine works. It helps by decreasing the reuptake of that catecholamine. That’s what I can say about ephedrine. It can be somewhat unpredictable how it can react in patients.
I would start off and maybe try 0.1 milligrams per kilo to start. I said that a couple of different times. You can always give more. Once you give it, you can’t take it back. Make sure that you are diluting it appropriately. It comes at 15 milligrams, and you want to dose it. In a good size adult, it’s 5 milligrams or 2.5 milligrams. On the kid, you want to make sure you are being very cognizant of the weight-based dosing, the 0.1 per kilo. I’d even go less than that sometimes to tell how they are going to react.
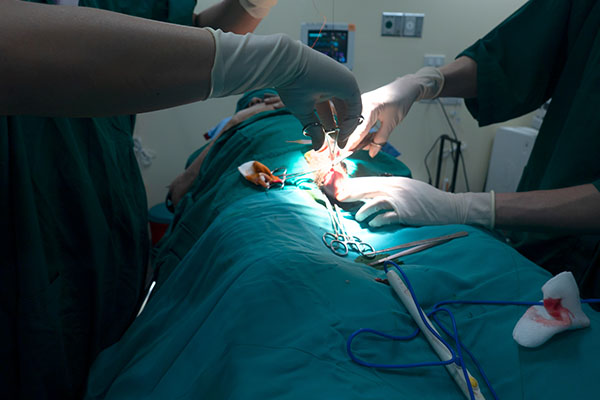
Cardiac Pharmacology: Vaso is a potent vasoconstrictor. It increases your arterial blood pressure. It’s a hormone found in the hypothalamus and sent to the poster pituitary, which is where it is released into the blood and can work in your kidneys to help reabsorb fluids.
That’s ephedrine. We are now going to go into the most common vasopressor that you are going to use. It’s going to be glued to your hand essentially in anesthesia. That’s neo. Everyone loves neo. You have NEO always ready to go, and it’s IV push. You can do a drip. That’s fine, but I’m going to go over the IV push because that’s 9 times out of 10 how you are going to use it in anesthesia.
A lot of hospitals now are doing these prefilled syringes, which is nice. It spoils you. Sometimes students get into the OR and don’t realize how to dilute it appropriately because they are spoiling you with pre-diluting things and putting them in your med drawer. You should always know how to dilute neo because it is an emergency drug. If you need it, you need to know how to use it and use it safely. If it comes in a 10-milligram vial, that is not safe.
This is just me, but I have seen people draw it up on a TB syringe. I have seen it done. If you do it safely and appropriately, that’s fine, but I don’t like that. I always dilute it in a 100 CC bag, or you can take 2 10 CC vials and double dilute it. That’s okay too, but make sure that you are getting 100 mics per ML. What you ultimately want is 100 mics per ML.
When you are giving neo, it’s an alpha-1. It causes arterial vasoconstriction. It’s very potent. It comes as a 10-milligram vial. Never push 10 milligrams at once. You can put 10 milligrams in 100 MLs. Back to some basic easy math, I like knocking off zeros. That’s my favorite thing to do. It’s so rewarding knocking off zeros when you are doing math.
If you have 10 milligrams in 100 MLs, if you knock off both those zeroes or if you are diluting it further down, now you are left with 1 mg and 10ml, which makes 100 mics per ML. That might have gotten a little confusing. Ultimately, you start with 10 milligrams and put it in 100 MLs. You are essentially diluting it down to make 100 mics per. You can also make it into 40 mics per. I have seen that also be the dose of choice. The 2 mcg per kilo is the dose per kilo (IVP) if you wanted to know that. It’s a common drug to use. It’s a great drug. You have to be careful with it. You want to make sure you are going slow with it and make sure you know how people are going to react.
Narcotics And Benzos
We are going to go on to narcotics and benzos, but I’m not going to go into all the different types of narcotics and benzos. We are going to go into fentanyl. In fentanyl, 1 to 2 mcgs per kilo are the loading dose. I like to do the one per kilo for intubation if it’s not going to be a stimulating case. Especially if you want to get them back breathing early on, I like the 1 mic per kilo loading dose, but you are not wrong to give 2 mic. Keep in mind how stimulating the case is going to be and how long you are going to have to wait before you have stimulation because you could deal with some hypotension because of it.
Fentanyl is a mu-opioid receptor. It binds the mu-opioid. Everything is compared back to morphine. When you are looking at narcotics, that’s how you can judge how potent it is. Fentanyl is 100 times more potent than morphine. Keep that in mind. Back to the open-heart scenario, we didn’t routinely use fentanyl for our open-hearts every now and then we did base on preference. You typically would give 1 gram of fentanyl prior to sternotomy. That’s a lot of fentanyl. It goes to show that it’s not nearly as potent as the drugs that I was used to using and like using, which was Sufentanil. What we would do when I would use fentanyl in my open-heart is a gram prior to sternotomy.
After intubation and going on a pump, you would start your mics per kilo per hour drip. That’s about 2 mics per kilo per hour of fentanyl. It’s typically what we would use in our open-hearts as a continuous drip. We would do Nimbex fentanyl. Fentanyl would be left out of the 2 mics per kilo per hour. We wouldn’t titrate it. We would still give the gram of fentanyl prior to sternotomy. That’s how we would do those cases. We would leave it on up until the very end of the case. It’s the same with the Nimbex.
The duration of action of fentanyl is 30 to 60 minutes. That’s probably all I’m going to share with you on fentanyl. You may or may not see fentanyl used in open-heart. It’s the most common drug or narcotic to use in open-heart. I found it to be more labor intensive. I saw a lot more ups and downs with my blood pressure with fentanyl versus using sufentanil. We are going to go to the sufentanil next.
Make sure you're always chatting with your attending CNA. Make sure you're coming up with a good game plan on how to do things, especially if it's your first day or first week. Share on XSufentanil, the duration of action is 30 minutes. It’s more potent but shorter acting for its peak effect. It seemed to be a little more forgiving. You could control it better and control the patient’s reaction to pain better with sufentanil. All you need to blunt intubation stimulation is 0.3 mics per kilo. It’s a very low dose to blunt the sympathetic surge you get with intubation. For open-heart, we would give anywhere from 25 to 50 mics for induction. It comes in a 250 mic vial or a 50 mic vial. If I was doing a carotid, for example, I could use sufentanil for a carotid. I wouldn’t do 250 mcgs for carotid, but I would get my 50 mcg vial. I would dilute it down to 5 mics per ML. You would maybe give 20 mcgs for induction and then maybe another 5 to 15 more mcgs throughout the rest of the case.
On average, you are giving anywhere from 35 to 40 mcgs for the entire carotid. It blunts the cough so they don’t wake up coughing and bucking. They are usually very comfortable. It’s a great drug for carotids. I don’t think a lot of people think about that. You have to be careful with it because you can’t get a lot of apnea. As long as you are dosing it appropriately and not giving it right before the end of the case, you are going to be fine. Giving someone 5 mcgs is not going to be so much that they are going to go apneic. If you are slamming them with 15 to 20 mics, you are going to get some apnea. Be cognizant of how to dose it, and you will be fine. It’s a great drug.
It can cause bradycardia, which, if you are in a heart, you don’t want them to have a fast heart rate. It will increase your cardiac demand. We welcome some bradycardia. Sometimes people got a little too bradycardiac in the 30s. Sometimes you would have to give a little bit of Robinul or ephedrine if they needed a blood pressure support medication. It’s a great drug for pain control. Sufentanil is about 500 to 1,000 times more potent than morphine. I know that’s a big range, but it probably depends on the patient and how they react to it. It gave me the range of 500 to 1,000 times more potent than morphine. It’s very potent. That’s all I have to share with you about sufentanil.
Let’s go on to midazolam versed, the most common benzo you are going to use in anesthesia. In an open-heart, we give anywhere from 5 to 10 milligrams. We typically gave 5 milligrams. I know a lot of institutions give 10 milligrams. That’s a lot. To think about it, a lot of these patients are older, or maybe have some renal insufficiency, and 10 milligrams could put grandma off her rocker for well over a week or more afterward. I try to think about these patients. Even though I know they spent some time in the ICU afterward, they are still going home within that week. Are they going to go home and fall? I always worry about falls and bleeds because a lot of the patients go home on blood thinners.
I get nervous using a lot of versed, especially in older people because the last thing you want to do is cause them to go home and fall and hit their head and have something else bad happen. Be aware of that. It’s a great drug. Don’t get me wrong. I like it, but you got to be cognizant of who you are giving it to and what the renal function is. Do you need that much? You are going to have gas.
What we did is we would give 2 or 3 for induction and 2 or 3 during the wake-up. When they are getting ready to come off bypass, we will give the other 2 or 3. I wait until they come off that way. I’d make sure it’s circulating to the pump because sometimes some of your drugs get stuck on the side of the tube from the cardiopulmonary bypass machine. That’s why I would wait. If you are cooling someone from an open-heart and warming them back up, you are going to increase your metabolic demands. Be cognizant of that and getting more versed for a case like that.
We typically didn’t cool all of our open-hearts. We would only do that if we did a circle rest case. Even then, we would only do the circle rest for a max of ten minutes. We would use Brevital, Decadron, or ice the head. Instead of Brevital, we would give a dose of propofol. Essentially, all you are trying to do is cause the isoelectric activity in the brain. It’s decreasing someone’s metabolic need to zero. They don’t have any thoughts going on in that brain. Be aware of how you are using it and why you are using it. Don’t slam someone with ton of versed and think that’s fine. We have whole 10 milligrams. You don’t have to use it all.
We would give 5 milligrams, but every place does it a little bit differently. Midazolam affects the GABA receptor, and the duration of action is 1 to 6 hours. That’s a big range. 6 hours versus 1 hour, what person are you? How much alcohol do you drink on a daily basis? This is broken out. The cytochrome P450, you are going to hear that a lot in your pharmacology courses and anesthesia. It’s how you metabolize a lot of drugs.
Patients who drink a lot of alcohol or take a lot of different types of drugs anyways at baseline tend to have more of this enzyme that breaks down our anesthetic drugs. Some patients are very sensitive to it. 1 milligram will make them amnestic. For other people, if you give 3 milligrams, they are like, “When are you going to start sedating me?” They are crawling out of their skin. With that being said, even patients who are acting like that, who are crawling out of their skin, I’m pretty quick to give them more as well, but at the same time, they may not remember being like that.
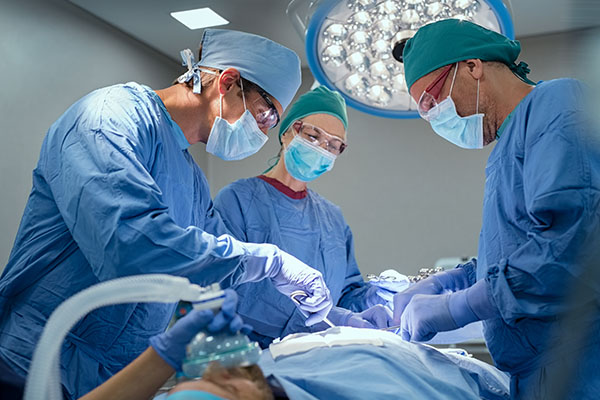
Cardiac Pharmacology: Fentanyl is a μ-opioid receptor. It binds the μ-opioid. It is a hundred times more potent than morphine.
Even though they are awake and interacting, they may be amnestic. Keep that in mind. It’s like being drunk but being awake. At the moment, you are aware of what you are doing, but the next day, you are like, “I don’t remember any of that.” That’s kind of how versed works a little bit. It’s probably the best relationship I can give you. Sometimes patients will be asking you, “When are you going to sedate me,” for a minor procedure, but you have to realize that. Even though they are acting like they are not sedated, chances are, they are not going to remember that.
Let’s get into it briefly because I’m not going to go into this a lot. This lecture has already been relatively long. Opioid sparing is an up-and-coming technique. It’s very widely accepted and used. It’s great. It has a lot of benefits for the patients. If you are doing an open-heart with an opioid-sparing technique, some of the things they do are usually do a regional block, which is one of the most common ones. This can vary based on where you do your rotation as the SAP, Serratus Anterior Plane block, to help block the sternotomy incision pain. They can also do a pectoralis nerve block. They follow what they call ERAS, which is not just an open-heart. It’s for a lot of different types of procedures.
What that stands for is Enhanced Recovery After Surgery. They are looking for ways to cut down on narcotic use because narcotics are not benign. They come with side effects, like constipation and ileus. There’s the addicting factor to it too. It’s overall not good for patients. They do things like lidocaine infusions. Lidocaine infusions are good for neuropathic pain. Lidocaine is a sodium channel blocker. By blocking your sodium channels, that leads to decreased pain generation. To put it in simplified terms, it pretty much weakens your peripheral nociceptors to pain and decreases your central excitability.
That’s how lidocaine infusions work. It has to be an infusion, a one-time bolus of lidocaine. Even though it does have some of those properties, it’s not going to give you the same effect as an actual infusion where you are keeping your concentration over a period of time the same. The infusion is what works the best for that. You then have your Gabapentin, which is also an anticonvulsant. Neuropathic pain decreases the excitability of the posterior horn of neurons, which are responsible for the stimulation of pain and modulation of pain. That’s how Gabapentin works. You have something like carbo-loading, which is not even medication at all. It’s carbo-loading. Why do they do that?
The patients who fast typically have insulin resistance. When they start eating again, it messes with their whole metabolic system. A brittle diabetic needs to be careful with carb-loading. There’s a limitation to it. By carbo-loading and not putting your body under that starvation stress, you are reducing your overall stress hormone response generation. That in itself can decrease pain. That’s why they do it for patients who are not brittle diabetics. You have your Tylenol and NSAIDs.
Keep in mind that Tylenol is not an NSAID. Tylenol is an antipyretic and an anti-analgesic, but it’s not an anti-inflammatory medication. It only affects your COX-2 receptor where you have your true NSAIDs like Toradol, which is a nonselective COX-1, COX-2 inhibitor. That is an anti-inflammatory medication. Another quick little tidbit is when you are giving Toradol, especially if you are giving 30 milligrams, and let’s say your patient is 60 years old. Be aware that Toradol is very hard on your kidneys. You can put someone into renal insufficiency with Toradol, especially if they are older. Decrease the dose. If you are going to give it, give 15 milligrams.
You can do a lot of harm with a whopping big dose of Toradol, like 30 milligrams. In a pediatric population, we do a 0.3 milligram per kilo dose. That’s how we dose it. For an adult, sometimes we get so used to giving standard doses. We don’t think about it. Be aware of that. Be also aware that if you are over 50 years old, you should start to think about, “Should I be decreasing the dose? Even though they can handle 30 milligrams, maybe she will only get 15 milligrams because it’s not a benign drug.”
You then have ketamine, which is an NMDA antagonist, especially if you are giving ketamine in small doses. A preventative dose for pain is anywhere from 50 milligrams to start and then maybe work another 10 or 30 milligrams throughout the case to wake up. Even if it’s not 50 milligrams, maybe start it with 30 milligrams and titrate in 10 more milligrams throughout the case for a total of 50 or 60 milligrams. That’s still a small enough dose. You shouldn’t get crazy nystagmus or anything crazy when you wake up.
I still caution you in using versed. That’s a good idea to still use a little bit of versed if you are giving ketamine because there can be hallucinogenic effects with ketamine. Who wants to wake up crawling on the ceiling? I don’t. Please don’t do that to me. I don’t want to itch my skin off because there are ants crawling all over me. It can have those potential side effects. Be aware of that.
Narcotics are not benign; they come with side effects, constipation, and ileus and are addicting. It's just overall not good for patients. Share on XYou typically get that more with an induction dose of ketamine, but it still can happen with low doses. You also have Precedex, which is an alpha-2 agonist. It essentially reduces substance P, which is a neurotransmitter that modulates pain. Substance P is Pain. It works by decreasing your norepi circulation too. It might not cause bradycardia, but it can cause hypotension.
It’s also very interesting. You can have transient hypertension with Precedex, especially if you are giving a bolus of it. I saw that. It does happen. It’s extremely rare, to be quite honest. No one that I was even with that date had ever seen it before, including myself. That actually can happen too. Be aware of that. Precedex is not a benign drug. You got to make sure you are giving it slowly when you are giving a bolus load of it. That’s the gist of how it works. I know I threw a lot at you guys. I tried to condense it into quick little tidbits to not overwhelm you with everything. I hope I covered everything in good enough form.
I tend to be the person who goes back to things sometimes. I’m like, “Did I say that right,” because I’m speaking quickly, and I don’t know. There’s one thing I want to go back to real quick because I’m not sure if I said this correctly. The last thing I want to do is confuse anyone here. I’m going to go back to my neo and the 10 milligrams and 100 MLs. 10 milligrams is 10,000 mcgs. Whenever you are figuring out head math, you want to think about, “How many mcgs am I giving?” 10 milligrams is 10,000 mcgs.
Let’s go back to the whole deletion of zeros. If you write down 10,000 and write down 100, and if you cross off two 0’s and two 0’s on both ends on the 100 and the 10,000, you are left with 100. 1 CC is 100 mcgs. I don’t know if I thoroughly explained that or if I got anyone confused. That’s the last thing I want to do. I want to back and make sure I went over that. I’m always here if you have questions. Reach out to me. I know it was heavy, but I hope you guys enjoyed it. I hope it helped somewhat clarify things in what you are in store for if you are ready to start your open-heart rotation. That’s super exciting. I hope you guys enjoyed it and have a fabulous day.
—
As always, I appreciate you and your loyalty. Thank you so much for reading. I’d love to learn from you, so screenshot this episode and share your IG Stories with your biggest takeaway. Don’t forget to include the #CRNASchoolPrepAcademy. If you are on Facebook, be sure to follow on IG or TikTok at @CRNASchoolPrepAcademy
Important Links
Get access to planning tools, valuable CRNA Faculty guidance & mapped out courses that have been proven to accelerate your CRNA success! Become a member of CRNA School Prep Academy here:
https://www.crnaschoolprepacademy.com/join
Book a mock interview, resume edit or personal statement critique:
Join the CSPA email list: https://www.cspaedu.com/podcast-email
Send Jenny an email or make a podcast request!









