
ICU sedatives and paralytics can look similar on the surface because both can make a patient appear calm and still, but they are not interchangeable. In this faculty led session, Dr. Matthew Harmon breaks down the real difference between sedation and paralysis, why it matters for patient safety, and how to avoid the most common clinical mistake, assuming a paralyzed patient is comfortable.
Get the Free CRNA School Data Sheet!
Compare every CRNA program’s requirements, deadlines, and interview details—all in one organized spreadsheet. The CRNA School Data Sheet helps you filter programs by ICU experience requirements, GRE, CCRN, last 60 credit GPA, and more so you can build a smarter school list without the confusion.
It’s updated regularly by the CSPA team, making it the easiest way to research and track CRNA school requirements. Bookmark it, plan your next steps, and finally feel confident that you’re staying on top of every requirement.
Access it free here: https://community.crnaschoolprepacademy.com/crna-school-requirements-spreadsheet
Join Us for Gassed Up: Fired Up for CRNA School The CSPA 2026 Conference
June 12th – 14th at the University of Louisville, KY
Ticket and Agenda Information: https://events.crnaschoolprepacademy.com/
Want Guaranteed CRNA School Admission? Learn how CSPA’s Personalized Money-Back Guarantee sets you up for success: https://community.crnaschoolprepacademy.com/6-12-month-intensive
Get access to application & interview preparation resources plus ICU Educational Workshops that have helped thousands of nurses accelerate their CRNA success. Become a member of CRNA School Prep Academy: https://community.crnaschoolprepacademy.com/join-cspa
—
Watch the episode here
Listen to the podcast here
Meet Dr. Harmon, DNP, CRNA, CSPA Faculty Coach and Assistant Program Director
Welcome to the CRNA School Prep Academy Podcast, where we have helped guide more than 10,000 ICU nurses on their path toward CRNA school. Our mission is to combine education, guidance, and professional growth so you can move confidently toward your goal of becoming a CRNA.
Whether you are still in nursing school or you are a seasoned ICU nurse, this podcast is here for you.
In today’s episode, you are listening to one of our faculty-led sessions streamed live on CSPA’s Instagram. Depending on the night, this may be an open Q&A where we take your questions in real time, or a focused topic discussion where we go deep on an area that can strengthen your knowledge and build your confidence.
If you want to follow along and join us live, make sure you are following CSPA on Instagram and watch for session announcements. You can also join CSPA’s free community, where we share the schedule of upcoming sessions. When you tune in live, you can ask questions, get clarity on the spot, and learn alongside other nurses navigating the same path.
As a quick reminder about who you are learning from, every session is led by CSPA coaches and faculty who are deeply committed to your success in pursuing this career.
Without further ado, let’s get into today’s episode.
—
Hello. Welcome to today’s live session. My name is Dr. Matthew Harmon. I have over eight years experience as a CRNA and have been involved in CRNA education and admissions since 2020. I’m one of the faculty coaches and mentors with CRNA School Prep Academy.
So just a couple general housekeeping rules for tonight. Okay. This is going to be a session topic, so what we’re going to do is I’m going to talk about sedatives and paralytics, a little bit knowing the difference, some things that are very good for ICU practice and care, but also are important for anesthesia. Additionally, we rotate through TikTok and Instagram for our live sessions with CRNA School Prep Academy. And you can learn more about our upcoming in-person conference at CRNA Schoolprepacademy.com. That’s going to be in Louisville, Kentucky in June 2026. You can join our free community through the link tree in our bio. And let’s jump into this topic now.
Why Sedatives vs Paralytics Matters
When we talk about sedatives versus paralytics, it’s important to understand the difference and use them intentionally. Anytime a patient can’t move, it’s incredibly easy for us as providers to assume that somebody is comfortable, but that’s not always the case. Paralysis can hide that pain, that fear, and that awareness. Sometimes you’ll see that in your vital signs with tachycardia and hypertension. Other times, if the patient is very ill, you might not see that.
So we’re gonna focus today on indications and timing for these drugs, good drug combinations and some rationales, monitoring tips, red flags, and then of course, reversal considerations. Because if you’re heading into CRNA school, you’re gonna be asked a lot about these drugs, and it’s important that you demonstrate your knowledge that you can go above and beyond.
Sedation Basics and Key Terms
So when it comes to sedatives, sedatives are going to alter consciousness, they affect our brain. And you’re gonna hear some terms used, and some of these are used interchangeably, but you need to know the difference.
Anxiolysis. When a drug is an anxiolytic, it’s going to reduce anxiety. If a drug is an amnestic, it prevents the formation of memory. If a drug provides some hypnosis, this can induce sleep and unresponsiveness. And if we’re using drugs that provide analgesia, you may think of narcotics, opioids, fentanyl, ketamine and Precedex provide some analgesia. However, propofol does not.
Common ICU and Anesthesia Sedatives
Now, getting into some of our sedative drugs, propofol, it’s a GABA-A agonist. It has a very quick and rapid onset. The duration of action is actually fairly short, somewhere between five and ten minutes. It does not give any analgesia. So you, if you have a patient who is uncomfortable, you need to pair it with an agent that is going to provide some pain control. Propofol has some anti-emetic properties, it can lower ICP, reduce cerebral metabolism. And the reason why its duration of action is so short is it works by redistribution because when you inject propofol into a vein, very quickly does that drug circulate around, go to the brain, and very quickly will it redistribute. And that’s why it has that short duration of action.
Another drug you may see used as a sedative in the ICU is midazolam, okay, or Versed. Versed being a versatile sedative. Midazolam is a benzodiazepine. It’s going to give good anxiolysis. It’s going to give good amnesia. All right. It’s not going to give retrograde amnesia. It’s not going to make you forget what’s happened, but the moment you give it, you get that anterograde amnesia. So going forward, those memories become harder to form. Versus, and a lot of the benzodiazepines, minus rhyming masolam, that’s a very anesthesia-specific drug, but the majority of benzodiazepines have very long context-sensitive half-lives. They accumulate. They’re not really reliable for deep sedation or a very rapid and brisk wake up.
Ketamine is used in sometimes the ICU and a lot in anesthesia. It provides a dissociative type of anesthetic. Ketamine is a unique drug because it works on our NMDA receptors. It’s an NMDA antagonist. And so what’s unique about ketamine is, and you may have seen this in the ICU, but ketamine can be used to help preserve those airway reflexes, that respiratory drive. It can give some analgesia. It’s great in asthmatics, it has some bronchodilatory properties, and it can increase your heart rate, your blood pressure. There’s a little bit of research on talking about increasing that ICP unless they’re well sedated. But ketamine is a very useful drug, and we use it a lot in anesthesia.
Dexmedetomidine, this is a selective alpha-2 agonist. I love Precedex. Love Precedex and anesthesia. Funny, I didn’t really like it in the ICU. Because at that time, and I was in the ICU many, many years ago, 2012, 2013, Precedex was oftentimes used by itself, and now I think it’s paired a lot. But it gives that sedation-like natural sleep. It’s not a respiratory depressant, which is very useful in anesthesia. It’s great for somebody who needs some help, being comfortable on BIPAP, maybe somebody who’s going through alcohol withdrawal, weaning vent modes, great, great to use.
Precedex, slower onset. You give that bolus dose, that one mic per kilo, over 10 minutes, and you’re gonna see that bradycardia. It also causes transient hypertension. I said Precedex is an alpha-2 agonist. It has a specificity for the alpha 2 to alpha 1 receptor of about 1600 to 1, while clonidine, another alpha 2 agonist, is much less, that 200 to 400 to 1. So when you rapidly bolus Precedex, you may have seen this, you may not. You’ll really see it if you have an art line in, but you’ll get transient hypertension. Okay? So that pressure will go up and very quickly will go down. It takes about a minute for it to hit because you lose specificity because you’re bolusing so much, so you’re gonna affect your alpha receptors as well, and then it will very quickly go back down, and then you’ll see that bradycardia.
Paralytics Basics and Core Safety Warning
Now, let’s talk about paralytics. Paralytics are going to stop that skeletal muscle movement, but they don’t do anything to the brain. The scariest thing you can ever have is a patient who is paralyzed, but they can hear, they can feel, they can remember, but they can’t respond. Paralytics give no anxiolysis, no amnestic, no pain control.
There are two types of paralytics or muscle relaxants. Depending on who you’re talking to, sometimes whenever you’re giving report in anesthesia and you say, Oh, we paralyzed and reversed them, patients will really, what happened? So many times what we say is muscle relaxants. You have two types. You have depolarizing and nondepolarizing.
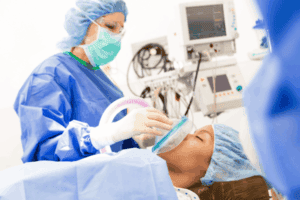
Mastering ICU Sedatives: When it comes to sedation, sedation changes the brain. Paralysis changes the body. Sedation is going to create that anxiolysis while paralysis is going to stop you from moving.
Common Paralytics and How They Work
The only depolarizer we routinely use is succinylcholine. And it chemically is two acetylcholine molecules joined together. It mimics that action of acetylcholine, it will depolarize and it will stay attached until it dissipates away.
The nondepolarizers, and you have steroidal like rocuronium, you also have cisatracurium or Nimbex. They competitively block acetylcholine at those nicotinic receptors. All right, and you all are probably very familiar with cisatracurium or Nimbex.
Succinylcholine should only last a couple minutes, it has a duration of about five to ten minutes, and it has a very, very quick onset. We use it for rapid sequence inductions or intubations. And there are some risks with succinylcholine. It’s not benign. There it can be a malignant hyperthermia trigger, which is, you know, a pharmacogenetic disorder that can lead to patient death, and is something we talk about in anesthesia that’s associated with our volatile anesthetics as well. Succinylcholine can also cause a rapid increase in your potassium, can cause hyperkalemia. It’s contraindicated in patients who have burns, crush injuries, have been laying in the bed for days on end because your extrajunctional receptors can proliferate, and then whenever you give succinylcholine, it will cause a huge amount of potassium to leak outside and cause that hyperkalemia.
Now, rocuronium, this is probably one of the paralytics I use the most. So it’s a nondepolarizer, it’s a steroidal. And you can always remember the steroidal muscle relaxants because they’re gonna be rocuronium, vecuronium, pancuronium, I would say rhonsomroids. So that’s a good way to remember the steroidal muscle relaxants.
Quick onset, 45 to 60 seconds. You can use it in a place of succinylcholine as your RSI dose. And then it can last approximately 35 to 70 minutes, and it can be reversible with sugammadex or neostigmine. Sugammadex is a completely true reversal, kind of how protamine can encapsulate that heparin molecule. Sugammadex encapsulates that rocuronium molecule. All right. Neostigmine was the older rev we would call it a reversal, but it’s not really a reversal, it’s competitive antagonism and had a lot of bad side effects.
Cisatracurium or Nimbex, so this is great because it has a little organ independent elimination. As long as somebody is warm, as long as somebody is given enough time, Nimbex metabolizes pretty quickly. All right, you can’t use sugammadex for it. It’s great for liver or renal failure patients, and it’s often used in a prolonged, extended stay. But it’s great for paralysis.
Sedation vs Paralysis in Practice
Now, when it comes to sedation, sedation changes the brain. All right, paralysis changes the body. Okay, sedation is going to create that anxiolysis while paralysis is going to stop you from moving. So if you see a paralyzed patient and their heart rate increases, they go from a normal sinus rhythm, a heart rate of 75 to 80, to 120. What could that mean? Could that mean pain? Could that mean panic? Could that mean hypoxia? Could that mean all three? All right.
When you think of paralysis, all right, you need to be giving some anxiolysis, some pain control. So there are times where you don’t need paralytics, you just need sedation. What are some examples of this?
- Ventilator tolerance. Sedation will decrease that anxiety, that dyspnea.
- Severe anxiety, okay, for patient comfort.
- Maybe somebody has a very elevated ICP, propofol can decrease your CMRO2. That’s cerebral metabolic rate of oxygen consumption.
- Alcohol withdrawal, Precedex is great for it. It decreases those catecholamine surges and seizures.
- It is a wonderful, some of the sedatives do. Propofol can suppress that cortical activity, benzodiazepines are very commonly used in seizures.
So, what are your sedation goals? All right, you’re very familiar with the RASS scores, negative one to negative two, to help with that ventilator tolerance. And if you want that deeper sedation, a RASS of negative four to negative five, preventing ICP spikes, severe respiratory failure, things like that. In anesthesia, sedation is rarely the only plan, especially in airway manipulation. All right.
Now, when might we use paralysis? So paralysis is all about mechanics and not comfort.
- It’s great for that rapid sequence induction to prevent those reflexive glottic closures to make intubation easier.
- Paralysis is great in ARDS. We need to get those low tidal volumes in, that’s strict control.
- Proning is very, very useful.
- Controlling ICP so there’s no coughing, no shivering, or refractory event dyssynchrony, all right, to remove that muscular effort.
- If you can’t get somebody to tolerate the ventilator, you need to sedate them and then you can relax them or truthfully paralyze them.
So the order matters, sedation, then paralysis.
All right. You want to see that patient’s respiratory drive, that’s just because we’re talking about an intubated and ventilated patient. You want to see that respiratory drive, you want to see that ventilator be able to work. Think of that ARDS patient. Okay, so you may have to treat that pain, you may have to treat that discomfort with not only a sedative, maybe a narcotic for pain control, and then a paralyzed patient. But you never want to have somebody who is just getting a paralytic. That’s why in anesthesia we use a balanced approach.
And so we think of anesthesia with multiple needs. Do we need amnesia? Do we need anxiolysis? Benzodiazepines can be very useful. Do we need hypnosis or sedation or induction drugs? Propofol, very, very commonly used. Do we need pain control? Opioids, ketamine, dexmedetomidine helps prevent pain and reduce opioid consumption. And then if we need somebody immobile for a procedure, we’re going to use a paralytic or a muscle relaxant.
Now, some very common combinations of drugs you’ll see is your RSI combinations, propofol and rocuronium. That rapid sequence induction, no coughing, fast on, fast off, great in the OR, great in the ICU. That hemodynamically unstable patient. Maybe we’re going to use etomidate. All right. Etomidate can help preserve that blood pressure and heart rate. Sometimes it’s ketamine as well.
If you’re using succinylcholine, okay, rapid airway control, maybe that patient has the full stomach. All right. But do they have any contraindications for succinylcholine? Because if you give enough rocuronium, it will have almost as quick of an onset as succinylcholine, but without those dangerous side effects.
Ketamine and rocuronium, great for that asthmatic. Maybe somebody who is somewhat hypotensive because ketamine will help maintain that sympathetic tone, but you really need to make sure that patient has catecholamine reserves.
And then Precedex, a wonderful drug. It’s not a paralytic, it’s not an opioid, it’s the alpha-2 agonist, and it can help reduce your opioid consumption. It’s great for sedation. Anytime you do an awake fiberoptic intubation, I love Precedex. I give it to almost every anesthetic. It’s great for pediatric wake-ups, for vent weaning, things like that.
What might be your go-to ICU combo, all right, for your RSIs? You’re probably seeing propofol and rocuronium, ketamine and rocuronium.
Monitoring, Safety, and Reversal Considerations
Now, when it comes to monitoring for paralysis, some very important questions.
- Is that patient adequately sedated? And are you seeing vital signs to reflect that?
- How are you infusing these drugs?
- If it is a peripheral IV, you need to make sure that it is actually in, that it is running. Because if you’re giving low dose through a peripheral IV, it may take hours before you see that it is infiltrated.
- This is why it’s great if you have a central line, check it, make sure that you are using it.
- Is the airway manageable if something changes?
- If you’re if I’m there in the ICU about to intubate somebody, I need to have not only a plan A, but a plan B and a plan C for managing that airway.
- If I can’t get that airway, what am I going to do? How am I going to breathe for that patient if I paralyze them?
- How do you handle hypotension after you give these drugs?
- Is the vent right there dialed in?
- Do you have an Ambu bag?
- Do you have everything you possibly need?
Now, when it comes to monitoring for sedation, some people use the bispectral index monitor, the BIS monitor.
- 40 to 60 is going to be that anesthetic level state.
- 60 to 80 is going to be that good sedation state.
- When you start seeing 20 to 40, all right, when you start seeing 0 to 20, you’re talking about almost an isoelectric line, heavy, heavy sedation.
Tachycardia, hypertension. These can be signs of pain, anxiety. This can be a patient that is too light. Okay? Anytime you see lacrimation or tearing, all right, that is a sign that that sedation was a little light. All right. Maybe you even see them wincing. Remember, a paralyzed patient cannot tell you that they’re hurting, but their autonomic system still can react.
How do you monitor neuromuscular blockade? Oftentimes you use the train of four monitor. In the ICU, a lot of times we’re looking for one to two twitches. In the OR, we like deep paralysis. Okay? Typically, no twitches to one twitch, where the majority of those receptors are blocked.
Now we don’t want deep paralysis for so long that we have to give extremely high doses of our reversal agent, but there are consequences for not enough neuromuscular blockade on board. In the ICU, all right, this is someone fighting the vent, coughing. In the OR, this is a patient moving. Maybe a laryngospasm with light anesthesia during LMA use. Anything like that can happen. So we have to be very conscious of the drugs we use.
When we remove that movement from the patient, we can remove feedback. So we want to monitor them. We want to make sure that they are safe.
And a few things to mention for thinking about these drugs. What are the reversals for them?
- For our benzodiazepines, we have flumazenil.
- For our opioids, we have Narcan or naloxone.
- Propofol doesn’t have a reversal agent, it’s time.
- Ketamine is the same way.
- Precedex is the same way.
You have to use some caution with flumazenil and benzodiazepines if they’re a chronic benzodiazepine user. Naloxone or Narcan can cause that catecholamine surge, can cause pulmonary edema.
For your paralytics, sugammadex for your steroidal, or neostigmine. For your non-steroidal. Alright. Neostigmine, once again, not a true reversal. It works by competitive antagonism.
And cisatracurium in the ICU oftentimes is turning off for time.
And succinylcholine, all right, is metabolized by pseudocholinesterase. So someone can be pseudocholinesterase deficient. And succinylcholine can go from lasting five to ten minutes to twenty to thirty, to sometimes hours and hours.
Remember, sedatives are going to affect the mind, paralytics are affecting the body and the movement. They’re different tools for accomplishing different goals. And it’s very important that you understand the safety with them. Alright?
So whenever you are thinking about coming into anesthesia and practicing as a CRNA, it’s important that you understand these drugs. And the best way to understand these drugs is to do what you’re doing now, working in the ICU.
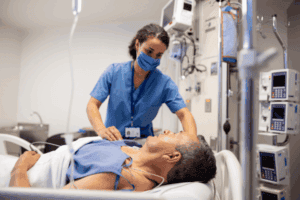
Mastering ICU Sedatives: If you are working toward CRNA school, understanding sedatives and paralytics matters. The best way to build that knowledge is exactly what you are doing right now, taking care of patients in the ICU.
Questions and Answers
So I’m gonna go back through, add a couple of things in the chat, and then we’ll open it up to some QAs. Alright? Oh yeah, my shirt, it says Synesthesia. So I own Synesthesia CRNA. I do we have a company that does education tracking, and we use it for CRNA programs to track your evaluations, your cases, things like that.
All right. Any questions in the chat for me related to ICU or any of the topics we talked about today? It’s important to remember that whenever you have patients that are receiving these medications, that you are monitoring them.
Question: What is my favorite anesthesia drug and why? What is my least favorite?
Honestly, I think my favorite drug is Precedex. I love dexmedetomidine. Why? It’s smooth wake up. Patients just do really well with it. Whenever I think about formulating an anesthetic plan and postoperative goals, I’m gonna think about a patient who is back to themselves, who’s relaxed, who doesn’t have much anxiety, and that’s why.
My least favorite, you know, I never take a drug out of the out of the toolbox completely. There’s always an indication for one. I would say my least favorite, and it’s not truly an anesthetic drug, but it’s metoclopramide or Reglan. You know, it’s a gastric prokinetic. It makes some people very, very anxious and it can cause them a lot of anxiety. It it was a very old school thing, you would give it before C-sections, and by the time you left the labor room, got them into the OR to put in their spinal, they’re even more nervous. So I don’t really like giving Reglan unless there’s that true indication for it.
Question: Why am I checking CK whenever my patient’s on a propofol drip?
So there’s a syndrome, propofol infusion syndrome, whenever you give propofol for extended periods of time. All right, propofol has lipid content in it, and it can cause some interesting side effects whenever given for a prolonged period of time.
So you’ll see in the ICU, we will look at caloric intake from propofol. We will look at we’ll monitor urine because it can change the color of the urine, and we’re gonna monitor how much of other changes it may have whenever it comes to not only your kidneys, but your liver, anything like that, whenever you have that extended amount of propofol sedation. Normally that happens after a day or two or super, super high injection, super high doses.
Question: Why why injections succinylcholine is not used these days?
Succinylcholine has honestly fallen out of favor. The bad side effects, it gets a bad rap, it causes a lot of muscle pain. The myalgias from succinylcholine can be very, very severe. And sometimes you’ll hear what’s the myalgias are often related to fasciculation. So when you give sux, if you don’t give what we call a defasciculating dose, you’ll see their muscle spasm. Okay, and it can be very, very intense. And patients have a lot of discomfort afterwards.
Question: Any golden rules specific to peds versus adults with anesthesia?
Certainly. When it comes to kids, kids can be very, very challenging. All right. You need the highest anesthetic requirements in a person comparatively, six months to one year, all right. Oftentimes kids need a much higher dosage relative to their body weight. Okay? And so we’re always using weight-based dosages as well, but kids you have to keep deep. You have to be very careful with waking them up. Kids can laryngospasm. And there are stages of anesthesia. And that stage, there’s four we talk about stage two is that hyperexcitability, that’s the most dangerous that’s when a child can laryngospasm. So with kids, wake them up or keep them deep. All right, don’t try to extubate them in between.
With adults, I would say my biggest thing is pay close attention to your vital signs and look at your end-tidal CO2. Your end-tidal CO2 can be a good representation of your cardiac output. So if suddenly your end-tidal CO2 drops, you’re automatically thinking, okay, hey, my patient’s cardiac output has dropped, they are not, they’re not doing well, that’s why my blood pressure cuff is cycling so much, or maybe my A-line’s alarming, my pressure’s dropping, I need to correct it immediately.
Question: What would be a good advice to prep for CRNA school? What book can you recommend to start getting ahead of the game?
That’s a really good question, but I tell people this once you’re accepted into CRNA school, don’t do anything except keep taking the challenging patients in the ICU and take some time off before you start CRNA school. Have a little time for yourself.
If you are bound and determined to read anything, I think a good EKG book is really useful. You’ll get into studying anesthesia. I wouldn’t read more than about it than you want to. If you’re bound and determined to study anything, anesthesia, I think the Basics of Anesthesia, I think this is by Miller and Pardo. One of the easiest books to read. It’s a great intro to all things anesthesia.
Question: What type of complications have I faced in my practice before intubation or after extubation?
I’ve seen anything and everything. One of the most scary complications is somebody who’s a full stomach, or maybe somebody who lied about their NPO status, or it’s an emergency, and we have to intubate them anyways, and they begin to vomit. And so trying to prevent aspiration, you know, if you can’t get the airway right away, things like that. So those are things that can be very complicated. Or after extubation, making sure that person is awake, making sure I leave them in care of the PACU nurse in a safe state, making sure that they’re not having any complications.
All right, we’ve got about five minutes left.
Question: Qualifications to become CRNAs.
So CRNAs are advanced practice registered nurses. So the United States are primarily aware of CRNAs practice, like, I don’t think there’s another country that truly has the practice model that we have in the United States of giving all types of anesthesia and being involved in every aspect of it. You would need a bachelor’s degree, at least a year of critical care experience, and then it’s a three-year program where you’re going to do hundreds and hundreds of cases, spend thousands of hours in the OR, and become really, really good at all types of things, anesthesia.
Oh, the Basics of Anesthesia is the name of the book. If you think any of the EKG books, if you just read like a page or two a day, keep it on your nightstand, it will dramatically change how you’re able to look at and interpret your EKGs.
Question: Would you move to a level one if you live only by level two hospital?
You don’t have to. As long as you’re taking sick, critically ill patients that are intubated, sedated, that have pressure requirements, that you’re dealing with art lines, central lines, other bedside procedures. If you can, if you’re in a CVICU where you see swans, things like that, you’re right where you need to be.
Question: Is it possible to work a shadow in the ICU prior to passing the NCLEX while studying for your BSN?
Hung, did you work in the ICU before CRNA school? Totally. I would hope most nursing schools have you do a rotation there. And you should be able to pick, you should be able to pick your ideal place to precept in the ICU. So if you’re able to do that, spend your time there. This way you can see if that’s where you want to be. The ICU is challenging. For me personally, I had I started applying to school right at a year and got in pretty quickly after that. So by the time I started CRNA school, I had almost two years.
Question: What is my personal preferred approach on induction for trauma patients?
Trauma is very challenging. It depends on the type of trauma, depends on what I’m there for. If they’re already intubated, all right, I just need to take them to VOR, get them sedated. If I’m called, if I’m called to the ER to help intubate a trauma coming in, thinking about vital signs, I’m thinking about securing the airway quickly. Oftentimes it’s ketamine and rocuronium because I don’t if I don’t know their history, I’m very cautious with just getting succinylcholine blindly. And then I’m gonna get secure their airway, probably very quickly have respiratory start suction them out while I have things set up for an art line, and then this way I can monitor blood pressure if we’re doing CPR and you know then start making sure I have adequate access. Because normally they’re gonna come in with like at least one IV or an IO or something. If it’s you know hemorrhagic trauma, you know, maybe I’m gonna get nine French in the neck to where we can rapidly infuse pretty quickly.
Question: Can you explain steroidal versus non-steroidal paralytics, just how they are metabolized?
So you have your steroidal and your non-steroidal. Non-steroidal would be like cisatracurium or atracurium. Those are metabolized by Hofmann elimination. Okay, so really independent of much liver or kidney involvement, your steroidal are going to have some type of liver or renal involvement. And so for somebody that has very, very complex issues, a lot of times in the ICU we prefer to use cisatracurium or Nimbex so you can just turn it off. Now in the OR, 99.9% of the time I’m using rocuronium because I have a true reversal for it, and very quickly I can go ahead and give roc to intubate, it will last about the procedure and reverse it at the end.
All right. You guys asked some excellent questions. All right, always enjoy doing this. Follow CSPA on both platform or on all platforms, Facebook, follow us on Instagram, TikTok. We really love the good communication in these live sessions. Get on our website at crna schoolprepacademy.com. Check if you can make it to the conference in Louisville in June. It would be phenomenal. We’d love to meet a lot of you there. And really enjoyed the QA and shout out to Synesthesia CRNA, like I said, my company that is support anesthesia education software. Thank you all so much and have a wonderful rest of your day.
Related Topics to Explore
What Is A CRNA? How Do You Become A CRNA? Plus CRNA Salary Information and the Top 10 Best CRNA Programs! – Learn what CRNAs do, how to become one, and what salary and program details matter most before applying.
CRNA School Cost: A Comprehensive Guide to Paying for CRNA School — Explore realistic costs and financing options for future CRNAs.
Why Your CRNA School Interview Matters Most – Discover why your interview can make or break your CRNA application and how to stand out when it counts.
CRNA School Competition: How Hard Is It To Get Into CRNA School? – Understand what makes CRNA admissions so competitive and how to rise above other applicants.
Why Choose CSPA Over Other Prep Programs? – Learn how guidance rooted in real CRNA admissions experience helps remove the guesswork and gives you clarity tailored to your unique & specific goals, background, and timeline.
Important Links
Join the Free CSPA Community! Connect with Aspiring CRNAs, Nurse Anesthesia Residents, practicing CRNAs, and CRNA Program Faculty Mentors who are ready to support you. Get real answers and expert guidance in a welcoming space that’s free from misinformation and negativity. You don’t have to do this alone! Join Now: https://www.cspaedu.com/community
Get access to application & interview preparation resources plus ICU Educational Workshops that have helped thousands of nurses accelerate their CRNA success. Become a member of CRNA School Prep Academy: https://community.crnaschoolprepacademy.com/join-cspa
Want Guaranteed CRNA School Admission? Learn More about the CSPA Money Back Guarantee here: https://community.crnaschoolprepacademy.com/6-12-month-intensive
Get CRNA School insights sent straight to your inbox! Sign up for the CSPA email newsletter: https://community.crnaschoolprepacademy.com/email-sign-up
Book a mock interview, resume or personal statement critique, transcript review and more: www.teachrn.com













